

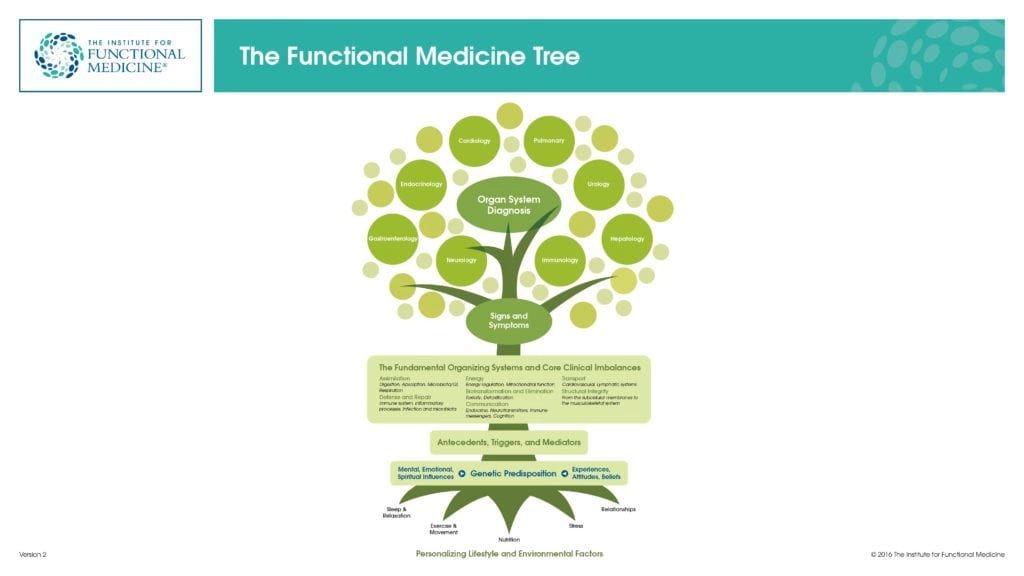
The mouth is, and forever will be part of the body. The old model in traditional medicine of treating symptoms and body parts in isolation, is flawed. Pioneers in functional medicine like Dr. Mark Hyman, Dr. Mike Roisen, Dr. Axe, Dr. Fuhrman, Dr. Amy Doneen, Dr. Brad Bale, and a host of others are leading the charge in functional medicine. They do not ask questions like “what do we have, “but rather”why do we have it.” They understand that the body parts and organ systems are connected via the bloodstream, the lymphatic system, endocrine system, gastrointestinal system, nervous system, and immune system. Separation of organ systems and body parts does not exist. They understand that what happens in one part of the body, affects the entire being. The mouth is just one example, albeit a very potent one. In order to get to the basis of inflammation, which is a key driver of metabolic syndrome, one must address all sources of inflammation in the body. The most common site of inflammation, the most easily observed, and importantly – the easiest to treat, is periodontal inflammation. Periodontal disease is not a local disease, as it is often treated. For instance, evidence suggests that periodontal changes are the first clinical manifestation of diabetes, as well as a significant risk factor for poor glycemic control.
In clinical practice, we are guilty of overlooking a host of other oral signs of diabetes beyond gingival/periodontal changes, such as salivary Finding the root cause of disease – it’s all connected dysfunction, candidiasis, taste interference, neurosensory disorders, and oral infections. Enamel changes are often the first clinical manifestation of silent reflux.
Periodontal pathogens and the subsequent inflammatory mediators go off-site throughout the entire body as is referenced in a variety of scientific, peer-reviewed literature. The consequences of periodontal disease are widespread and often devastating. Ignoring this premise and the emerging research is putting our patient’s health and possibly their lives at risk. Therefore, it is up to all of us as healthcare providers to look for the signs and document changes, then be able to communicate those findings with patients. The mouth is the very best arena for identifying physical risk factors for obstructive sleep apnea, Xerostomia from polypharmacology influences, Caries, erosion, chronic gingival inflammation, and Candidiasis. Food sensitivities and allergies often show mucogingival manifestations before G.I. disturbances such as pain, bloating, diarrhea, or constipation and you just must be looking for those risk factors on every exam. As AAOSH team members, we have heard and read evidence-based research from scientists studying infertility and pre-term birth, heart attack and stroke prevention, cognitive decline and Alzheimer’s disease prevention, cancer prevention, metabolic syndrome prevention, and more. Every scientist has shown data that if we don’t treat underlying inflammation, we will not have long-term successful outcomes of systemic disease.
This is a profound time in healthcare reform and it’s important to not only get informed on the latest knowledge and facts regarding oral systemic health but know what to look for and help our patients understand their role in treating and preventing disease.
Do you have questions about our approach to more complete and holistic dental care? Our patient coordinator is standing by, happy to answer any questions you have to determine if we are right for you.
Copyright © 2026 Whole Health Dentistry • Desert Ridge Medical Plaza 20950 North Tatum Blvd, Suite 300 Phoenix, AZ 85050 • Phone: 480.563.4141